Diabetes Prevention
Lifestyle Modification
In those at high risk for developing diabetes or who have prediabetes, insulin secretion may be adequate to maintain fasting blood glucose levels below 126 mg/dL but the process of insulin resistance is already present. Patients with impaired glucose tolerance should be counseled on the benefits of modest weight loss and increasing physical activity. Weight loss and regular exercise can reduce the risk of diabetes by 34-43% over the next 7-20 years in long term studies.
Drug Therapy
There is increasing evidence that very high-risk patients under age 60 years old with prediabetes may limit progression to type 2 diabetes by using metformin to target insulin resistance.
Summary
For patients with IFG or IGT prediabetes, the ADA consensus panel currently recommends lifestyle modification including 7% weight loss and moderate intensity physical activity approximately 150 min/week (such as walking).
The panel recommends lifestyle modification and metformin for any of the following groups of patients, especially those who are less than 60 years old, and with BMI >35 or prior GDM:
- IGT (strength of recommendation: A, clear evidence)
- IFG (strength of recommendation: E, expert consensus)
- A1C 5.7-6.4% (strength of recommendation: E, expert consensus)
| ADA Evidence Grading System for Clinical Practice Recommendations |
|---|
A. Clear Evidence from well conducted, generalizable RCTs that are adequately powered
B. Supportive evidence from well conducted cohort studies, or a case control study C. Supportive evidence from a poorly controlled or uncontrolled studies; conflicting evidence D. Expert consensus or clinical experience |
Follow Up Monitoring
Routine at least annual monitoring for the development of diabetes should be performed with A1C testing in individuals with prediabetes IFG/IGT being treated with metformin. Those who are not receiving drug therapy should be seen annually. These patients should also be assessed and treated for other cardiovascular risk factors (e.g. hyperlipidemia, hypertension, tobacco use). Follow up counseling is also important for success of lifestyle modification.
Signs and Symptoms of Undiagnosed Diabetes
Most individuals with undiagnosed diabetes are asymptomatic. Undiagnosed glucose intolerance and persistent hyperglycemia may eventually lead to classic symptoms of increased thirst, polyuria, fatigue, weight loss, and blurry vision. Acanthosis nigricans is a skin change that can occur in those with insulin resistance. Other signs may include obesity, evidence of metabolic syndrome or cardiovascular disease.
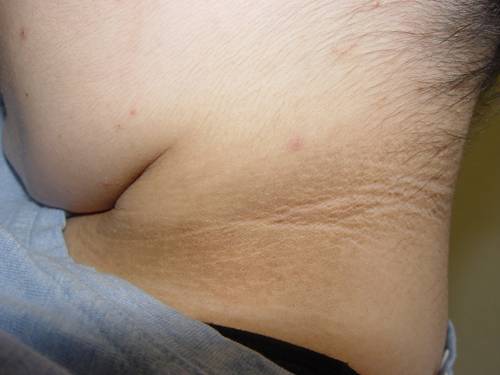
Acanthosis Nigricans from DermAtlas
Diabetes Care
The Initial Evaluation
As per the American Diabetes Association, the goals of a comprehensive medical evaluation in a patient with a diagnosis of diabetes are:
- to classify the patient
- to detect the presence of diabetes complications
- to review previous treatment and risk factor control in patients with established diabetes
- to assist in formulating management plans
- to provide the basis of ongoing care
Components of a comprehensive diabetes evaluation (ADA, 2014):
1. Medical history
- Age and characteristics of onset of diabetes (e.g., DKA, asymptomatic laboratory finding)
- Eating patterns, physical activity habits, nutritional status, and weight history; growth and development in children and adolescents
- Diabetes education history
- Review of previous treatment regimens and response to therapy (A1C records)
- Current treatment of diabetes, including medications, medication adherence and barriers to adhere to meal plan, physical activity patterns, and readiness for behavior change
- Results of glucose monitoring and patient’s use of data
- DKA frequency, severity, and cause
- Hypoglycemic episodes
- Hypoglycemia awareness
- Any severe hypoglycemia: frequency and cause
- History of diabetes-related complications
- Microvascular: retinopathy, nephropathy, neuropathy (sensory, including history of foot lesions; autonomic, including sexual dysfunction and gastroparesis)
- Macrovascular: CHD, cerebrovascular disease, and peripheral arterial disease (PAD)
- Psychosocial problems
- Dental disease
2. Physical examination
- Height, weight, BMI
- Blood pressure
- Fundoscopic examination
- Thyroid palpation
- Comprehensive foot examination: dorsalis pedis and posterior tibialis pulses; inspection; patellar and achilles reflexes; monofilament, proprioception and vibration sensation
- Skin examination (for acanthosis nigricans and insulin-injection sites)
3. Laboratory evaluation
- A1C
- Fasting lipid profile, including total cholesterol, HDL cholesterol, triglycerides, and LDL cholesterol
- Liver function tests
- Test for microalbuminuria
- Serum creatinine in adults
- Thyroid-stimulating hormone in all type 1 diabetic patients; in type 2 if clinically indicated or dyslipidemia or women >50
4. Referrals
- Eye exam–dilated exam
- Family planning for women of reproductive age
- Medical nutrition therapy (dietician)
- Diabetes educator
- Behavioral specialist, as indicated
- Dentist
Management
A physician-coordinated multi-disciplinary approach is recommended for providing care for patients with diabetes. Multi-disciplinary teams may include a physician, nurse practitioner, physician’s assistant, nurses, nutritionist, pharmacists, mental health specialists and a social worker. The individual with diabetes should assume an active role in their care in collaboration with the team. Care should be tailored for the individual’s needs and involve family and other support systems as allowed by the patient. All plans should recognize the paramount importance of diabetes self-management, patient education, and lifestyle modifications.